
Key Takeaways
- South Korea's AI welfare call system has already identified over 1,200 at-risk seniors who would have otherwise gone unnoticed, sparking global interest in AI senior monitoring.
- AI-powered health monitoring for seniors can detect early warning signs of cognitive decline, depression, and fall risk—but it works best alongside human caregivers, not as a replacement.
- American seniors living alone face a 26% higher risk of premature death, making proactive check-in systems a potential life-saving intervention for millions.
- Privacy, digital literacy, and equitable access remain the biggest barriers to widespread AI adoption in senior care across the United States.
A Startling Number That Should Change How We Think About Aging Alone
Here is a statistic that has stayed with me since I first encountered it in a 2023 National Academies of Sciences report: roughly 14 million Americans over the age of 65 live alone. Among those, an estimated one in four goes an entire week without a single meaningful human interaction. In my 22 years of practicing geriatric medicine, I have seen firsthand what that isolation does to a person’s body and mind—and it is far more destructive than most people realize.
Now, halfway across the world, South Korea is deploying something remarkable: an AI-powered welfare call system that phones elderly residents living alone, engages them in natural conversation, and flags potential health crises before they become emergencies. The results have been striking. Within its first operational year in select municipalities, the system identified over 1,200 seniors showing signs of severe depression, cognitive decline, or physical distress who had not been on any social worker’s radar.
The question I keep hearing from my patients and their families is straightforward: could something like this work here in the United States? The answer is nuanced, and that is exactly what this deep-dive analysis will explore—the real science behind AI senior health monitoring, the proven benefits, the legitimate concerns, and what American seniors should do right now to stay ahead of the curve.
What South Korea’s AI System Actually Does—And Why It Works
Beyond a Simple Phone Call
South Korea’s system, developed in partnership between municipal governments and domestic AI firms, is not a robocall. It uses advanced natural language processing to conduct weekly or biweekly phone conversations with seniors who have opted in. The AI asks open-ended questions about sleep, appetite, mood, pain levels, and daily activities. But the real innovation is what happens underneath the conversation.
The AI analyzes vocal biomarkers—subtle changes in speech pace, pitch variability, pause duration, and word-finding difficulty—that clinical research has linked to early-stage cognitive decline and depressive episodes. A 2024 study published in The Lancet Digital Health found that AI voice analysis could detect mild cognitive impairment with 83% accuracy, rivaling some in-person screening tools.
When the system detects a concerning pattern, it does not attempt to diagnose or treat. Instead, it routes an alert to a human social worker or community health nurse who follows up in person. This hybrid model—AI as the first line of detection, humans as the intervention—is what makes the approach so effective.
“The most dangerous health crises I see in older patients are the ones that develop slowly and silently—gradual cognitive changes, deepening depression, creeping malnutrition. By the time a family member or doctor notices, we’ve often lost months of intervention time. AI monitoring has the potential to close that gap dramatically.”
The Numbers Behind the Impact
According to data released by South Korea’s Ministry of Health and Welfare in early 2025, municipalities using the AI call system saw a 31% increase in early mental health referrals among seniors living alone and a 19% reduction in emergency hospitalizations related to falls and dehydration. Those are not marginal improvements. For context, a 19% reduction in fall-related ER visits across the American senior population would translate to roughly 570,000 fewer emergency admissions annually, based on CDC fall injury data.
South Korea’s demographic urgency—it has the fastest-aging population among OECD nations—forced early adoption. But the United States is not far behind. The Census Bureau projects that by 2030, every Baby Boomer will be 65 or older, creating the largest senior population in American history.
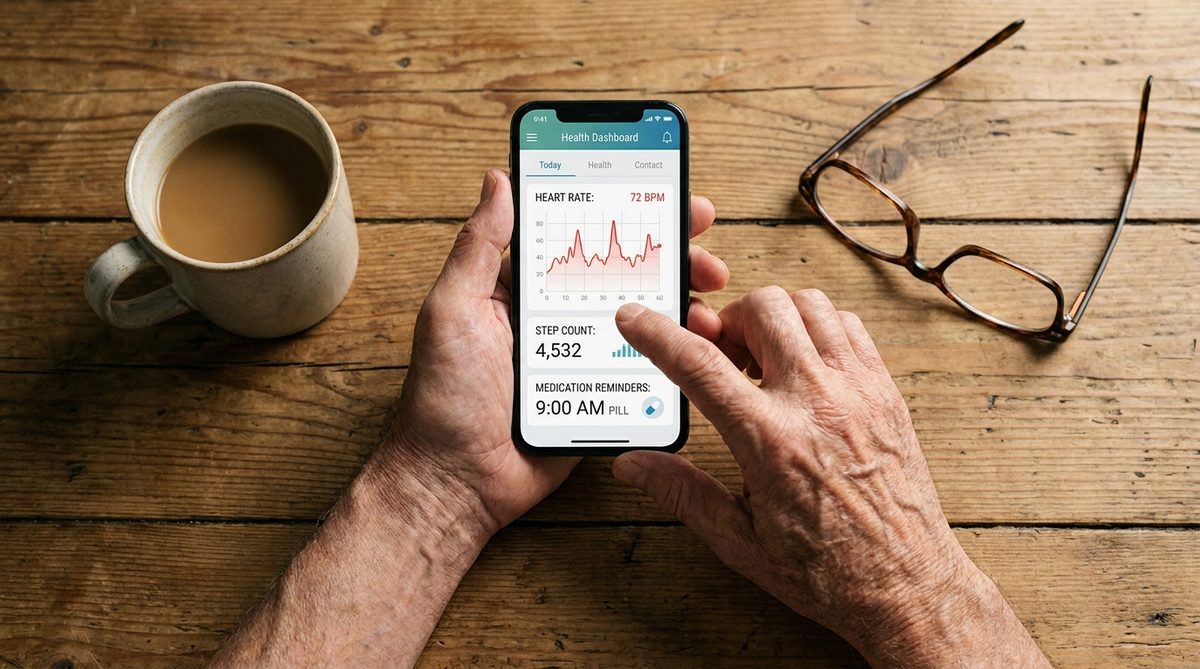
The American Landscape: Where AI Senior Health Monitoring Stands Today
What’s Already Available
While no U.S. municipality has replicated South Korea’s centralized AI call system at scale, the American market for AI-powered senior health tools has exploded. I routinely discuss these options with patients and their caregivers. The ecosystem now includes ambient monitoring sensors, wearable health trackers, AI-driven telehealth platforms, and voice-activated wellness check-ins through smart speakers.
The key distinction is that in the U.S., adoption is largely consumer-driven and private-sector-led, whereas South Korea’s model is government-funded and community-integrated. Each approach has trade-offs, which I’ve summarized below.
| Feature | South Korea (Government Model) | United States (Private/Consumer Model) |
|---|---|---|
| Cost to Senior | Free (government-funded) | $20–$250/month depending on service |
| Enrollment Method | Opt-in via social worker or community center | Self-purchase or family-initiated |
| Human Follow-Up | Built-in (social worker dispatched automatically) | Varies; some services include, many do not |
| Data Privacy | Government-regulated under national health data laws | Varies widely by company; HIPAA applies only to covered entities |
| Digital Literacy Required | Minimal (phone-based, AI initiates the call) | Moderate to high (app setup, device pairing) |
| Coverage Equity | Universal within participating municipalities | Skewed toward higher-income, tech-savvy seniors |
| Clinical Integration | Linked to national health records | Rarely integrated with primary care providers |
What I see most often in my practice is a frustrating gap: the seniors who would benefit most from AI monitoring—those who are isolated, lower-income, or cognitively declining—are the least likely to access it. This is the central equity challenge that any American implementation must solve.
Pilot Programs Worth Watching
Several promising U.S. initiatives are beginning to bridge this gap. The National Institute on Aging funded a 2024 pilot at three Area Agencies on Aging in Ohio, Texas, and Oregon that uses AI voice analysis during routine wellness calls already conducted by volunteers. Early results showed a 40% improvement in flagging seniors who needed follow-up compared to volunteer assessment alone.
Meanwhile, CMS (the Centers for Medicare & Medicaid Services) has begun evaluating whether AI-assisted remote patient monitoring for seniors with chronic conditions could qualify for expanded reimbursement under Medicare Advantage plans starting in 2026. If approved, this would be a game-changer for access, effectively subsidizing what is currently an out-of-pocket expense for most families.
If you’re exploring the broader technology landscape for aging in place, I recommend reading 5 Myths About Age Tech That Stop Seniors From Aging in Place, which debunks common misconceptions that prevent seniors from adopting tools that could genuinely help them.
The Clinical Case for AI Monitoring: What the Research Shows
Early Detection of Cognitive Decline
Alzheimer’s disease and related dementias affect approximately 6.9 million Americans aged 65 and older, according to the Alzheimer’s Association’s 2025 report. What makes early detection so critical is that the newest generation of disease-modifying therapies—lecanemab (Leqembi) and donanemab—show their greatest benefit when initiated in the earliest stages of cognitive impairment.
AI systems that analyze speech patterns, word recall, and conversational coherence over time can detect subtle changes months before a standard annual wellness visit would catch them. A 2024 meta-analysis in JAMA Neurology pooling data from 11 studies involving over 8,400 participants found that AI speech analysis had a sensitivity of 79% and specificity of 81% for detecting mild cognitive impairment—performance comparable to the Montreal Cognitive Assessment (MoCA), the most widely used clinical screening tool.
In my practice, I often tell my patients that the brain does not go from healthy to impaired overnight. There is a gradual slope, and the earlier we identify someone is on that slope, the more options we have. AI gives us the ability to monitor that slope continuously, not just once a year during a 15-minute office visit.
Depression and Social Isolation Screening
The link between social isolation and mortality is now as well-established as the link between smoking and lung cancer. A landmark Mayo Clinic review found that chronic loneliness increases mortality risk by 26%—equivalent to smoking 15 cigarettes per day. Among seniors, depression remains massively underdiagnosed; the CDC estimates that only about one-third of older adults with depression receive treatment.
AI check-in systems can track longitudinal changes in engagement—shorter responses, flatter affect, declining interest in previously enjoyed topics—and generate alerts before a crisis occurs. This is not theoretical. The South Korean data shows concrete reductions in suicide attempts among monitored seniors, a demographic that has the highest suicide rate in the OECD.
“Social isolation is not a lifestyle preference—it is a clinical risk factor. We screen for blood pressure, cholesterol, and blood sugar at every visit. We should be screening for isolation and loneliness with the same rigor, and AI gives us a scalable way to do that between visits.”
Fall Prevention and Medication Adherence
Falls are the leading cause of injury-related death among Americans over 65. Every year, roughly 3 million older adults are treated in emergency departments for fall injuries, and one in five falls causes a serious injury such as a hip fracture or head trauma. AI monitoring systems that incorporate motion sensors, gait analysis, or even simple daily activity tracking can identify increased fall risk—changes in walking speed, reduced movement throughout the home, or missed medication doses—and trigger early intervention.
Medication non-adherence is another silent crisis. The CDC estimates that poor medication adherence causes approximately 125,000 deaths and up to 25% of hospitalizations in older adults annually. AI-powered reminders with adaptive follow-up—not just a static alarm, but a system that escalates to a caregiver when doses are consistently missed—represent a meaningful step forward.
For a broader look at daily habits that complement these monitoring tools, 7 Healthy Aging Habits That Actually Work After 60 offers evidence-based strategies I frequently recommend to my own patients.

The Legitimate Concerns: Privacy, Trust, and the Human Element
Data Privacy Is Not a Minor Issue
Any system that continuously collects health-related data from vulnerable adults demands rigorous privacy protections. In the U.S., HIPAA applies only to covered entities—health plans, providers, and clearinghouses. Many consumer health apps and AI monitoring devices operate outside HIPAA’s reach, meaning your voice data, activity patterns, and health indicators could theoretically be shared with third parties or used for commercial purposes.
Before adopting any AI health monitoring tool, I advise my patients and their families to ask three critical questions:
- Where is my data stored, and who has access to it?
- Is my data encrypted both in transit and at rest?
- Can I delete my data completely if I discontinue the service?
If a company cannot answer these questions clearly and in writing, that is a red flag.
AI Cannot Replace Human Connection
This is perhaps the point I feel most strongly about as a clinician. AI is a powerful screening and monitoring tool. It is not a companion. It is not a caregiver. And it should never be used as an excuse to reduce human contact with isolated seniors.
South Korea’s model works precisely because AI is the detection layer, not the care layer. Every flagged concern results in a human visit. If American adoption focuses solely on the technology without building out the human response infrastructure—more social workers, more community health aides, more geriatric specialists—we risk creating an elaborate surveillance system that identifies problems but does nothing meaningful about them.
The Digital Divide Remains Real
According to Pew Research data from 2024, approximately 25% of Americans aged 65 and older do not use the internet. Among those over 80, the figure rises to nearly 40%. Rural seniors, low-income seniors, and those with disabilities face even steeper barriers. Any AI monitoring solution that requires broadband internet, smartphone proficiency, or complex device setup will systematically exclude those who need help most.
Phone-based systems like South Korea’s—where the AI calls the senior, not the other way around—offer the most inclusive approach. Voice is the most natural and accessible interface, and it requires nothing more than a landline or basic cell phone.
What American Seniors Should Do Right Now
You do not need to wait for a government program or a perfect technology to take meaningful action today. Based on the evidence and my clinical experience, here is what I recommend:
- Establish a regular check-in system. Whether it’s a family group text, a weekly phone call, or a structured volunteer visit through your local Area Agency on Aging, consistent human contact is the foundation of healthy aging.
- Explore AI-assisted tools cautiously. Smart speakers with health skill capabilities, wearable fall detectors with automatic alerts, and telehealth platforms with AI triage are all worth considering—but vet the privacy policies first.
- Talk to your doctor about cognitive screening. Ask your primary care provider about baseline cognitive assessments so that any future AI-detected changes can be compared against a known starting point.
- Advocate for public investment. Contact your representatives about supporting Medicare coverage for AI-assisted remote monitoring. The technology exists; the funding and policy framework do not yet match the opportunity.
- Stay physically and socially active. No technology replaces the health benefits of regular movement and genuine social engagement. For a science-backed framework, explore the 6 Pillars of a Healthier Age-Defying Lifestyle After 50.
The Road Ahead: Where AI Senior Health Monitoring Is Heading
The convergence of several trends makes the next three to five years critical for AI-powered elder care in the United States. The senior population is surging. The caregiver shortage is worsening—the Bureau of Labor Statistics projects a deficit of 446,000 home health aides by 2028. And the technology is maturing rapidly, with large language models becoming more capable of nuanced, empathetic conversation.
I expect to see Medicare Advantage plans begin bundling AI monitoring tools into chronic disease management programs by late 2026 or 2027. I anticipate state-level pilot programs modeled on the South Korean approach, likely starting in states with the oldest populations—Maine, Florida, West Virginia, and Vermont. And I believe voice-based AI will become a standard component of geriatric care plans within the decade.
But technology is only as good as the system it serves. If we invest in AI without simultaneously investing in geriatricians, social workers, community health infrastructure, and caregiver support, we will have built a very sophisticated alarm system with no one to answer the call.
The promise of AI senior health monitoring is real and backed by growing evidence. The responsibility to deploy it wisely, equitably, and humanely—that falls on all of us.
Frequently Asked Questions
Is AI senior health monitoring covered by Medicare?
As of mid-2025, standard Medicare does not cover most AI-powered health monitoring tools for seniors. However, some Medicare Advantage plans include remote patient monitoring benefits, and CMS is evaluating expanded reimbursement for AI-assisted monitoring starting in 2026. Check with your specific plan for current coverage details.
Can AI really detect early signs of Alzheimer's or dementia?
Emerging research shows that AI analysis of speech patterns—including word-finding difficulty, pause duration, and conversational coherence—can detect mild cognitive impairment with approximately 79-83% accuracy, according to studies published in JAMA Neurology and The Lancet Digital Health. It is not a diagnostic tool, but it can flag individuals who should receive formal clinical evaluation.
Are AI check-in calls safe for seniors concerned about phone scams?
Legitimate AI wellness call programs are opt-in, meaning you or a family member must enroll and consent before any calls begin. The calls come from a recognized number at a scheduled time. Unlike scam calls, they never ask for financial information, Social Security numbers, or passwords. Always verify the program through your local Area Agency on Aging or healthcare provider before enrolling.
What is the simplest AI health tool a senior can start using today?
A smart speaker such as an Amazon Echo or Google Nest Hub offers the lowest barrier to entry. These devices can set medication reminders, make emergency calls, conduct simple wellness check-ins through health-oriented voice apps, and connect with family members—all through voice commands with no screen or keyboard required. Setup typically takes under 15 minutes with family assistance.

About Dr. James Roberts, MD, Board-Certified in Geriatrics
Dr. James Roberts is a board-certified geriatrician with 22 years of clinical experience caring for American seniors. He specializes in chronic disease management, medication safety, cognitive health, and senior wellness. Dr. Roberts is passionate about translating the latest medical research into clear, practical guidance that helps older adults make confident, informed decisions about their health. At Daily Trends Now, his articles are based on peer-reviewed studies and authoritative sources such as the CDC, Mayo Clinic, and the National Institute on Aging.







